This post will show you how I do a single-unit dental implant. It’s not a cookbook, there are lots of great ways to get to the same result. This is just how I do it.
Hopefully it helps to see how different people work to give you ideas of your own.
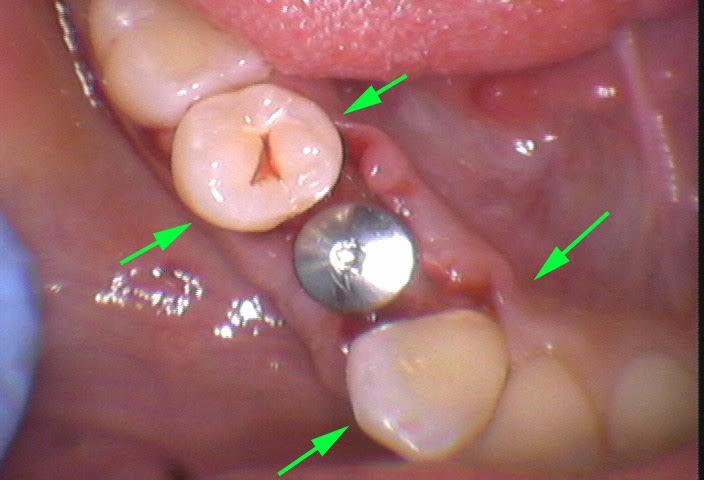
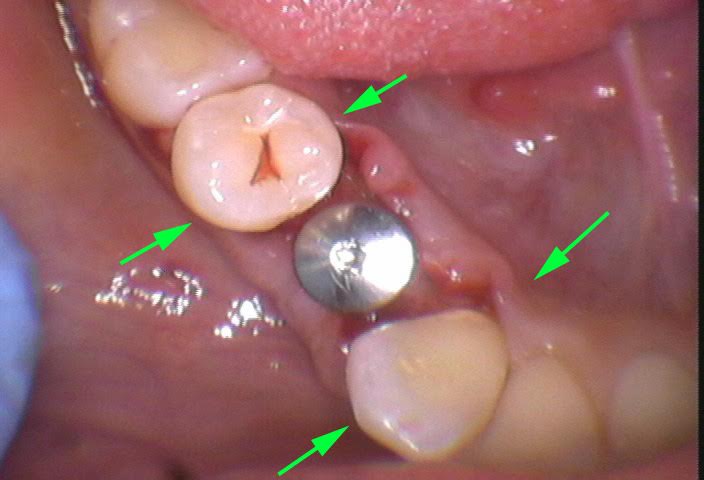
Internal resorption on a lower right 1st premolar.
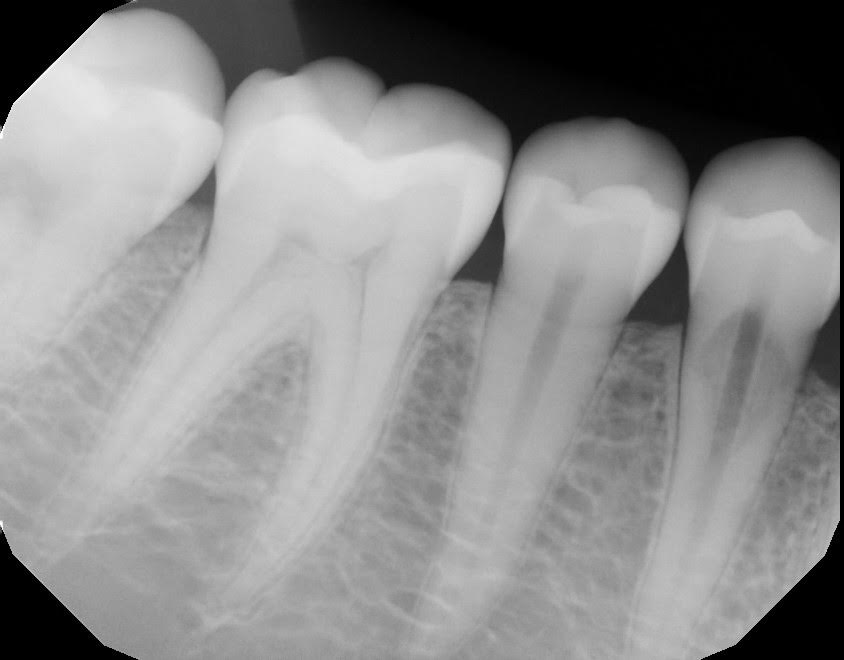
Which ultimately went to this: Straumann SLActive 4.1x12mm tissue level SP.
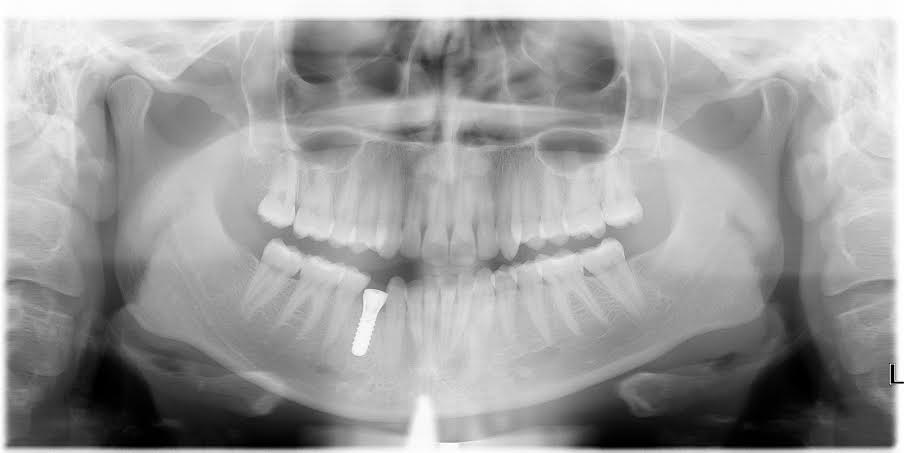
So there is internal resorption on the tooth:
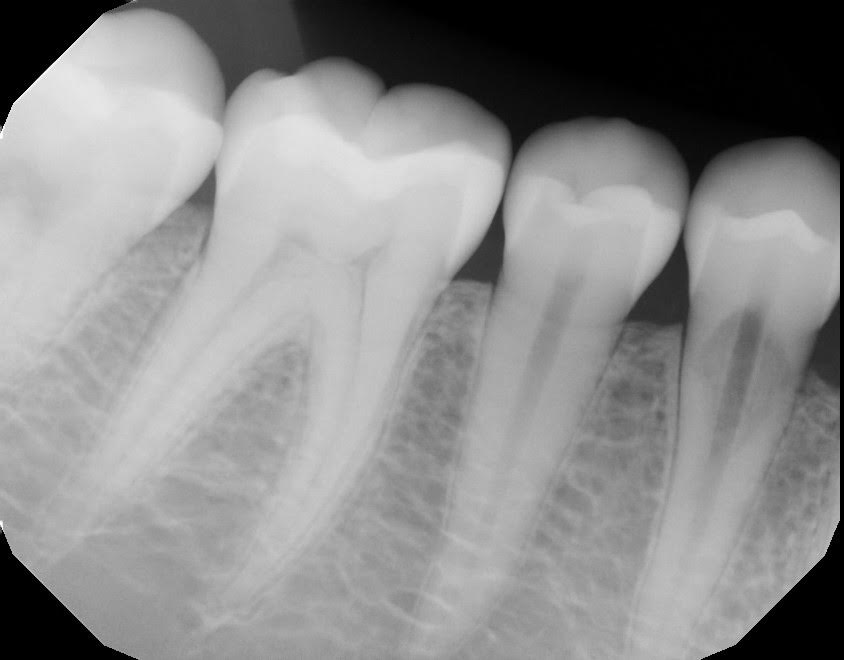
Diagnosis and Options
First this is referral to the endodontist, this is IMPORTANT, especially on a young pt (25-26 y/o). I’ve seen many times where endo want to monitor the tooth, however in this case, the endodontist recommended an extraction:
For those of you who are interested in learning more about external resorption here is a post I wrote that also includes some good clinical pictures of external resorption.
Choosing Treatment (pt needs to accept tx)
So after the endodontist recommended an extraction, I provided the patient an estimate and timeline of ALL options BEFORE an treatment is rendered.
This is very IMPORTANT.
Providing an estimate of all treatment options does a number of things for you.
(1) greatly increases case acceptance
(2) weeds out patients who are not interested, allowing you to spend more time with
(3) shows you provided a treatment plan to the patient,
(4) for the patients not ready yet, it gives them a reminder how YOU can help them

Creating and optimizing these estimate sheets from scratch was extremely time-consuming.
I am a big fan of utilizing systems and frameworks in my dental practice, so I designed a series of templates and spreadsheets. Now it is 2-3 minutes to provide the patient with a highly customized treatment estimate which I have found really boosted my case acceptance.
The other thing that helps, when providing patients with a customized estimate is, the ones that are not ready often come back 1-2 years later ready to do the work. I can’t explain it. Just something I noticed.
So a couple of tips.
Notice how I called it “implant placement” and not “implant surgery” ? I do my very best to avoid using the word surgery, unless in a rare case I am trying to discourage a patient from choosing that treatment option.
I also send the pt home with some other information I’ve developed, and there are a few key choice phrases I say to the patient.
I will include that information in a future Helpful Dentist Insider’s email.
So getting back to this case, the front desk then takes a copy of the estimate and scanned/timestamped into the pt’s chart. Helps cover you from a liability stand point, as well as increases patient acceptance.
So this pt decided to go ahead with implant surgery. First step is get the tooth out atraumatically.
Removed the tooth. Used periotomes and spade elevator. Socket preservation bone graft was not necessary. Buccal plate was intact.

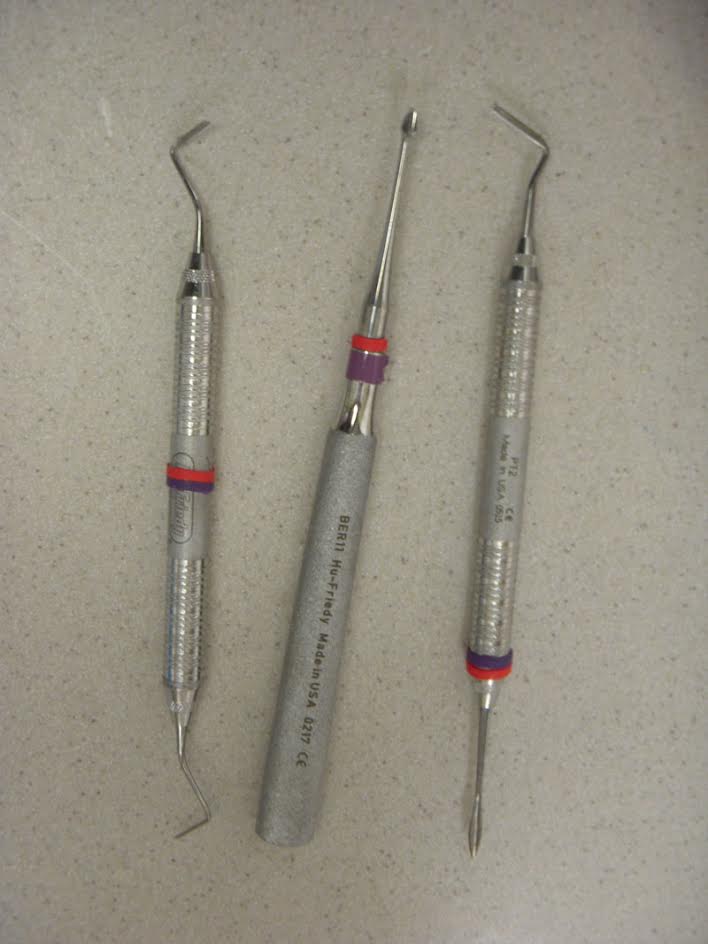

This is probably my favourite periotome: https://www.atitan.com/products/406-x-otome-straight
The spade is my absolute favorite elevator: https://www.atitan.com/products/24-straight-bone-preservation-elevator-%2363

For those who want to get a 10% discount on EVERYTHING at Atitan, I have negotiated an ongoing discount for the members. You have to use the checkout code “pearls10”. *Please note, I receive a commission on anything you purchase from Atitan using this discount code. These commissions help support the website and are appreciated very much. Thank you.*
Here’s more information on your 10% discount.
So there were no complications w/ the extraction. Kept buccal plate intact (which is important), verified with a perio probe, which meant there was no reason to do a socket preservation.
If you want to read a post I wrote on how I decide to bone graft or no bone graft, you can read those tips here.
Patient’s love this when I tell them the graft we planned on is not necessary because things went so well, and I personally find the bone tends to be harder if native bone. I sutured the area w/ gelfoam and figure-8 w/ 4-0 chromic gut as a precaution. Saw the pt back 3-4 days later at no charge in my 2nd treatment column for a post-op check (more on why this is a practice builder in another email).
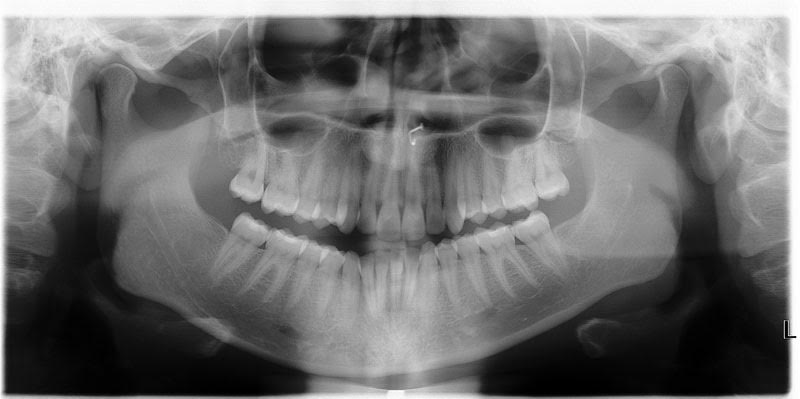
Waited and took a CBCT 11 weeks S/P exo reveals ample bone. Planned for surgery week 13:
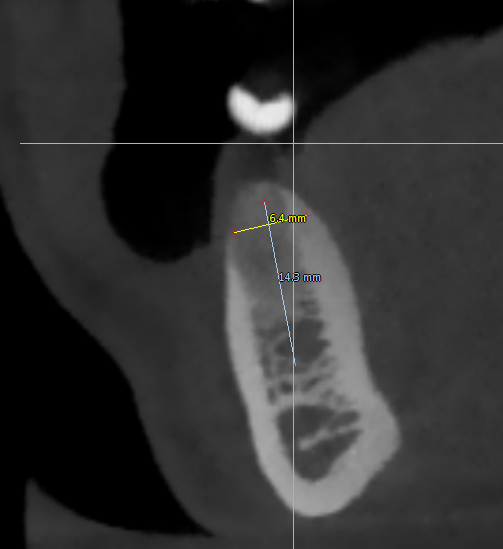
Make sure to locate the mental foramen on the tooth posterior, as well as the IAN loop. Here is a good post I wrote on this topic, for those who want to learn more.
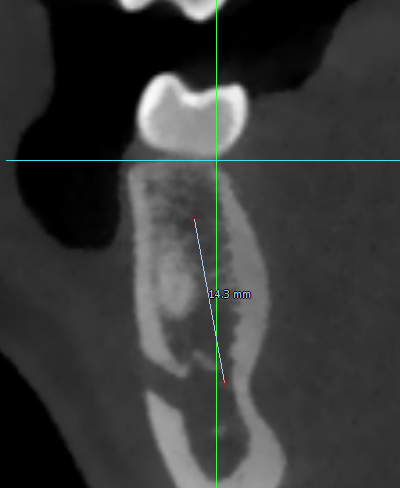
Planning the Case
The next thing I do is write your plan out a few days in advance. I still write these up for every implant case I do

I cannot stress this enough. Plan your cases out a few days in advance. Not the night before. Not the morning of. Definitely do not wing them. Plan your cases, ask questions to your mentors, take pictures, and study things IN ADVANCE.
The more complicated the case, the more steps I write out. Things like multi-unit, as well as sinus lifts, I literally write out each step by step. No shame in being over-prepared.
If there is one thing you take from this whole lesson, remember to plan your cases out and check inventory at least 3 days before the surgery.
I TAPE THE STEPS UP ON THE OPERATORY WALL BEHIND THE PT, SO I CAN REFER TO IT DURING SURGERY.
Inventory
VERY IMPORTANT: make sure you have the correct sizes of implants in stock, as well as cover screws and healing abutments. Give yourself at least 3 days of advance notice, so you can order parts if needed.

Hiossen has some great plastic containers that they will give you for free if you have enough volume or a hungry enough rep. This is how I organize my inventory.
It’s expensive to keep inventory, but it’s also more expensive to lose patient confidence over something simple. I like to keep 2 implant sizes of the common lengths at all times. Just in case something gets dropped, mishap, etc. Hasn’t happened yet, but I like being prepared.
The day you see the pt.
I take BP first. As long as the patient is healthy and ASA-I, personally, I will anesthetize the pt before the informed consent, so the patient is reading the informed consent while numbing up.
That’s a personal decision. You can decide to do how you choose.
IAN or Local Injections?
People ask me about my freezing for dental implants. I do a block on the lower jaw. Local + palate on the upper implants.
I like to do a IAN block. I plan my surgeries to have at least 2mm, and ideally more room to the IAN.
I’m aware of the folks who say if you do local injections the patient will feel it if you’re starting to get close to the nerve. I’ve tried this several times, and find patients hate all the injections and I end up doing a block anyway. I do a block. You can decide which approach you want to do.
Then in either situation (UA or LA), as long as there are not cardiac concerns, I go into the ridge and place Lido 2%, 1:50,000 for hemostatic control. I use it every time I lay a flap and semi-regularly when I take a crown and bridge impression.
Raise a Flap
I flap. I like to flap, and I like to see the bone as well as the bone quality of what I am working with. Tissue punches oses precious keratnized tissue, and surgically I cannot see unless I reflect the tissue. I did not take a picture of the flap reflection for this particular case, but I will provide some example images below.
What I typically like to do is a sulcular incision the mid-buccal and mid-lingual of the adjacent teeth. No releasing incision. In this particular case, I went to my usual mid-root of the opposing teeth buccal + lingual. I have a picture of the flap, but I don’t have one of the ridge. Sorry – can’t always take a picture of everything – I am working here at my day job.
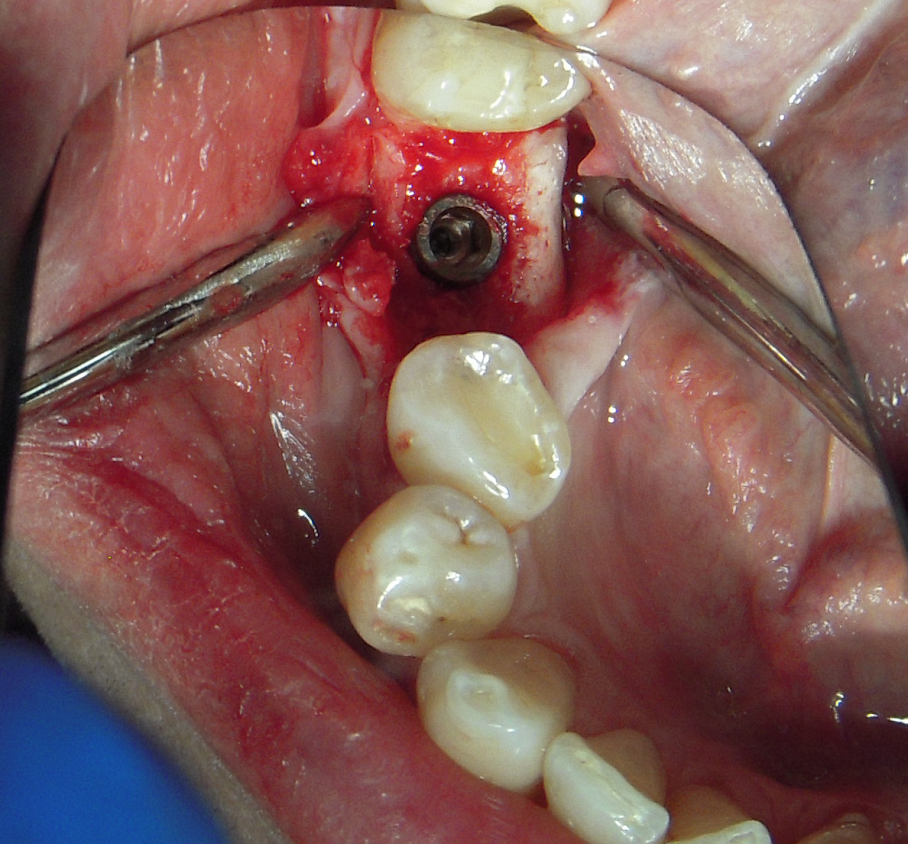
My assistant and I tend to use pritchards to hold the flap most of the time. We have 2. One for myself and one for the assistant. The majority of the time we use the small end.

You can also get pritchards at Atitan with your 10% discount (lowercase “pearls10”) here.
Different case, but lets you see the flap design. Notice you can visualize both the buccal (could be a bit more) and the lingual.
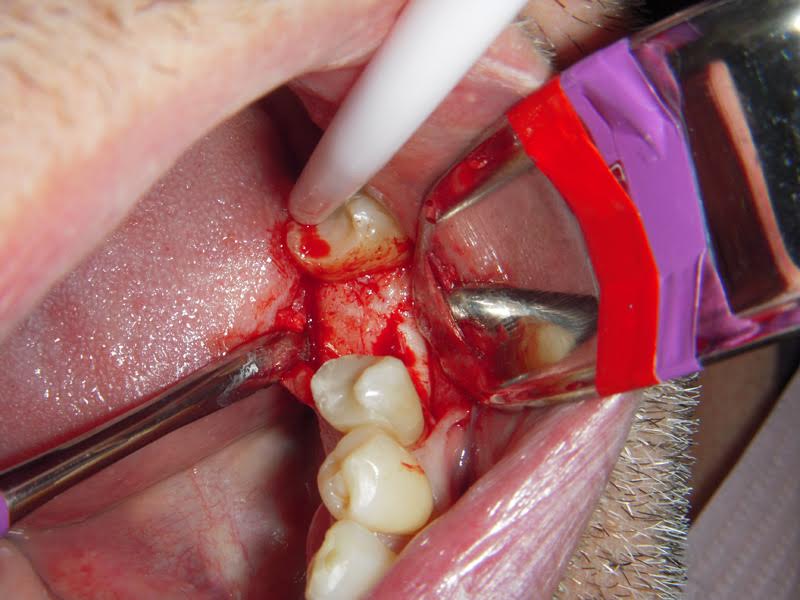
Here is a second different case. I flapped one tooth forward and one tooth back with no releasing incision. You get the idea. I like avoiding the releasing incision, as it keeps better vascularization, and sutures back easier. Better healing. With that said, I had a mentor who used to say “micro-flaps get micro-results.”
It’s important to have the flap far enough advanced you can SEE down both buccal + palatal/lingual walls
If you can’t see, you haven’t reflected enough
(keep in mind the buccal is very visualized, as the Minnesota is taking up space as well.)
Envelope flaps also tend to close up nicely.
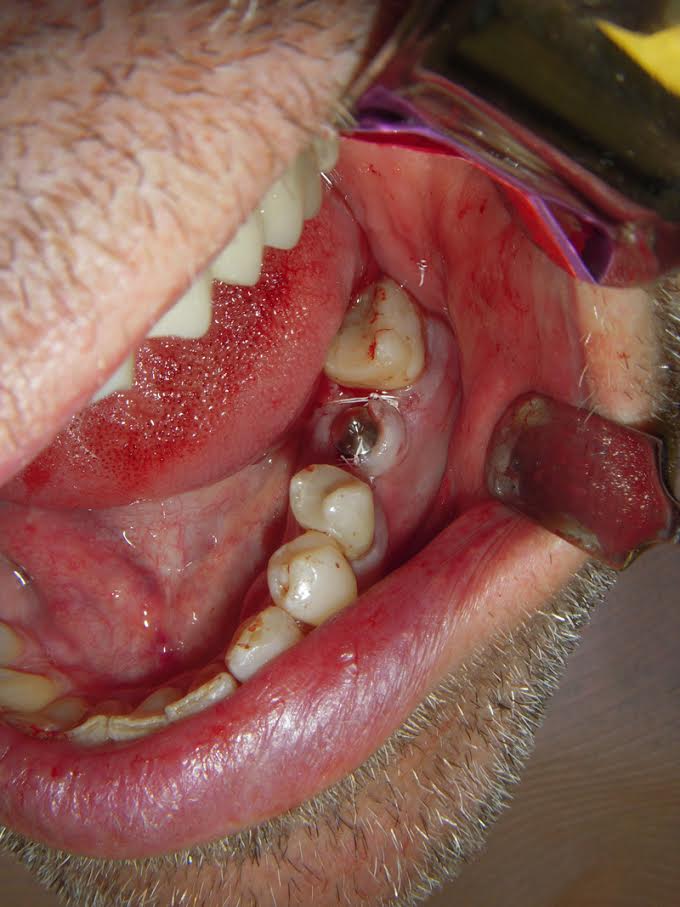
Tip: If you have trouble with too much tissue either buccal or lingual for your healing abutment, try marking the gingiva with a perio probe where you anticipate the implant going BEFORE flapping. I often do this when I have multiple units.
Preparing the Osteotomy
Once flapped, and verified I can see the buccal + lingual wall I use a 557 and a surgical handpiece to lightly score the bone where I intend to place the implant. I go in may 1mm. Just piercing the hard cortical plate.
I LOVE the MD guides (pictured below) but I find the MD drill skips around a LOT without a small pilot hole, so I use a 557 to remove a small circle of the cortical bone in the area I want my pilot hold to start.
Here is the MD guide. Have tried a few different techniques, and this one works best for my hands:
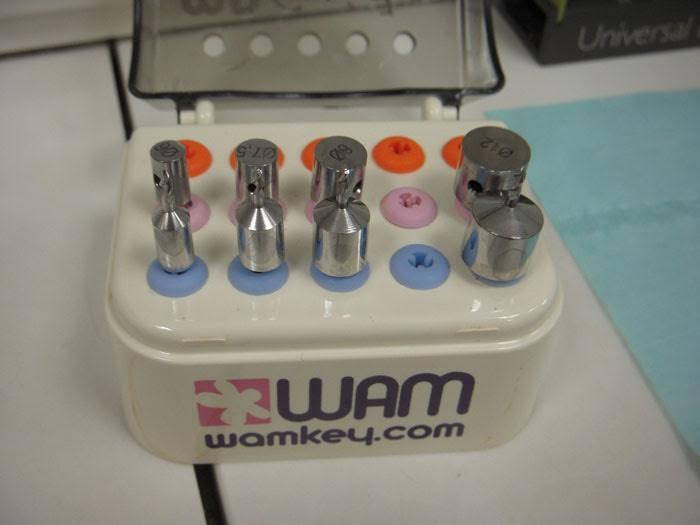
More info: http://www.wamkey.com/EN/produit/250-839/concept-
You can use the expensive lance implant drills, but a very amazing surgeon mentor told me the 557 trick, and it’s far more economical.
Basically BEORE using the MD guide drils, I prepare a small “occlusal” prep in the area where I want my pilot hole to go. This is to combat the skipping of the MD guide.
I’ve had a sabra for 5 years, use it every week, and it’s still working great.

It’s important to use a surgical handpiece and not a regular handpiece. A co-resident gave a family member of his an air embolism. We all saw the CT since the pt was worked up in the same hospital.
Here is an air emphysema case that goes into the importance of using a surgical handpiece.
After I have my 557 hole, just piercing through the cortical plate removed (say 1-2mm), I verify it’s position w/ a perio probe on the ridge. I look BL and MD w/ the perio probe. Turn the pt’s head and look at it from different angles. If my initial hole is in the area I want it to be, I then use my MD guide to go to 6-7mm. If not where I want to be, I make note of adjustments, and place another new hole.
Verify MD guide pin with a PA
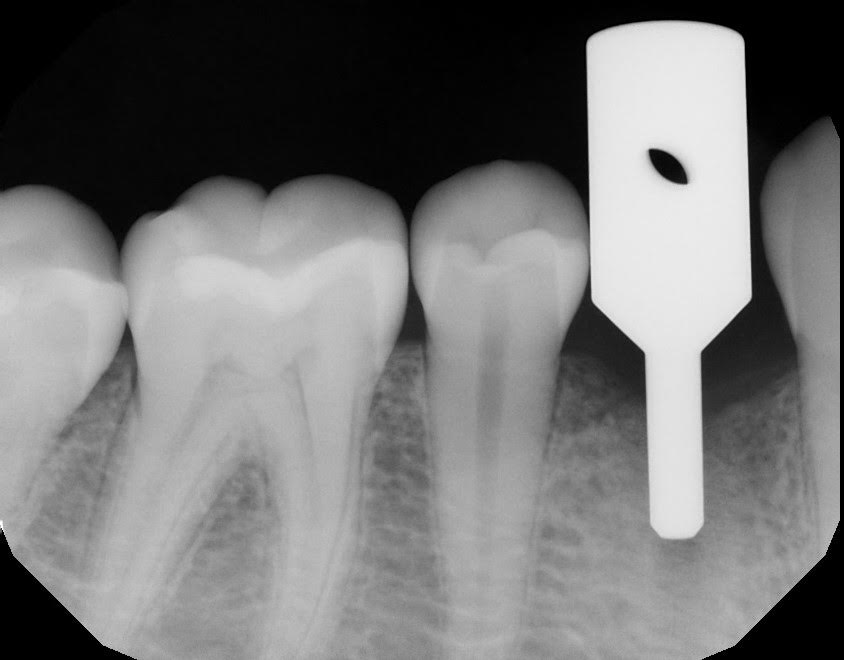
At this point, things are looking good. I know the MD guide, when fully seated is 7mm.
I have been using Versah densifying drills for about a year and a half now, and really like them. For this particular implant, after the MD guide PA I proceed to final depth of 12mm prepared for a 4.1mm diam Straumann tissue-level implant before taking another radiograph.
Angulation Tips:
Tip: I like to go to 6-7mm for a 10-12mm implant. It’s not long enough to hit an ajacent tooth, and doesn’t tear up the bone too much if angulation is really off and needs to be changed.
(1) If things are good after your angulation PA, proceed to depth and place the implant
(2) If angulation is good, but you’re concerned about depth, go to the full depth, and take a second PA, then place the implant
(3) If angulation is completely off, take a deep breath, turn the pt’s head, really suction off the site, look at it from all angles. Enlarge your flap, or do what is needed, then prepare the new osteotomy and KEEP IT AT 6mm to take another PA. If in this scenerio, then take another PA to the final depth (say 10mm) then a verification PA of the 2nd last drill size needed before placement.
Tip 2: It happens to everyone, but you can recover from an initial angulation issue if you haven’t drilled too deep. For example, here is a Hiossen 5x10mm I did last year that got myself off center. I’ve always liked the biohorizon 2mm drill, since it is very sharp, and has little notches that show the actual depth on the radiograph.
Straumann depth guide pins also have this. The more of these you do, the better you’ll get with less mishaps. The important thing is to always do your best to help the pt, recover from the error, and give them your absolute best effort. For me, drilling to 6-7mm at most helps me avoid any irreversible mistakes in my hands.
Here is an example early on in my career where I corrected my angulation because I did not drill too deep + checked my angulation.
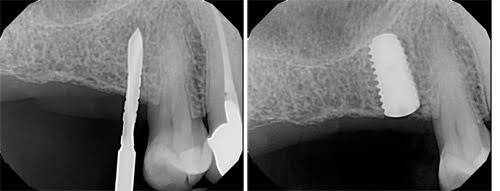
Densifying the Osteomtomy
I REALLY like the Versah densification burs. This is an old picture when I was first getting started w/ Versah, so I didn’t have all the drill sizes that I do now, but here’s the kit I put together w/ the Straumann parts I use the most.

more info: https://versah.com/densifying-reference-guide/
Here’s a good video:
For this case I was giving myself 14.5mm to the nerve. In cases where I do not have as much room I would likely have taken an x-ray at my backup length of either 8mm or 10mm, then decided if I wanted to proceed to 12mm. In this case, however, it was not necessary
Actual Implant Placement
Tip 4: before placing the actual implant, get a good guide-pin that shows depth markings. PUT THE GUIDE PIN IN YOUR OSTEOTOMY FIRST, and VERIFY THAT YOU ARE AT THE DEPTH YOU EXPECT TO BE AT, before putting the implant in.
I cannot tell you how many times I drill to 10mm or 12mm, or think that I did, only to put my depth pin in, and realize I’m 0.5mm short and have to drill a little deeper.
I like the Straumann pins, since they have the markings and easy to read measurements, and have clear markings that show up on the radiograph so you can easily verify depth.

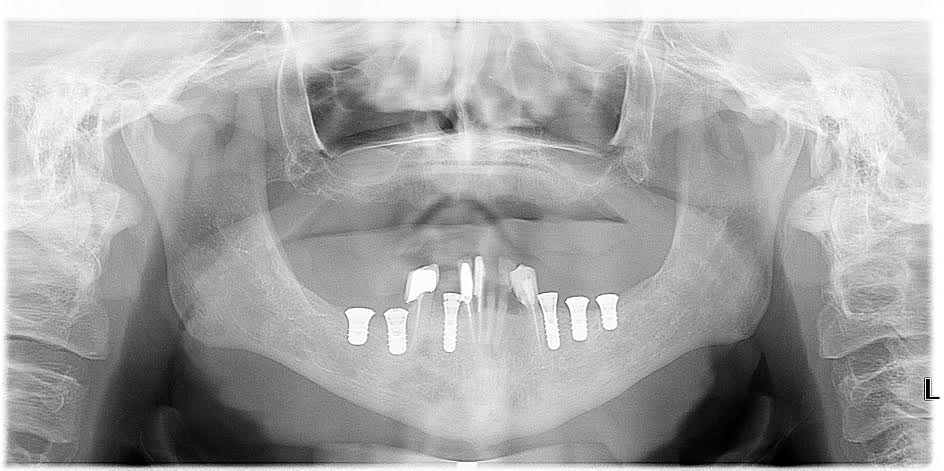
Example – see how I’m using the depth pins to check, before I place the implant? Notice how I’m short on 2 of the implants? I went back.
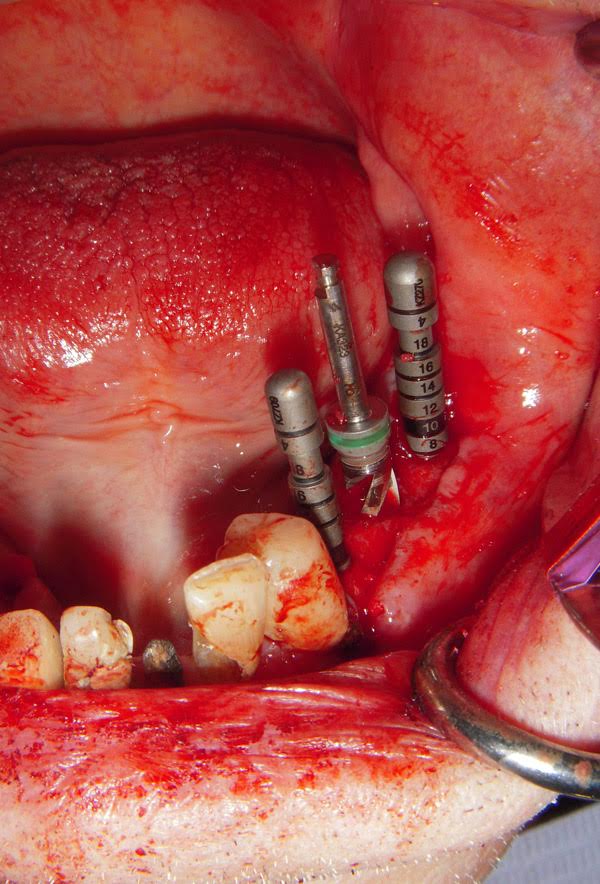
Here is how this case finished up a while ago. For those wondering why some compromised teeth were left, I placed 6 implants. I like to let them heal, and once the implants osseointegrated, I will impress for a temporary hybrid, extract all the pt’s teeth and deliver temporary hybrid for 8-12 weeks before finalizing the prothesis.
CBCT showed a large undercut on the posterior region, hence it looking like I had more vertical bone than I actually did.
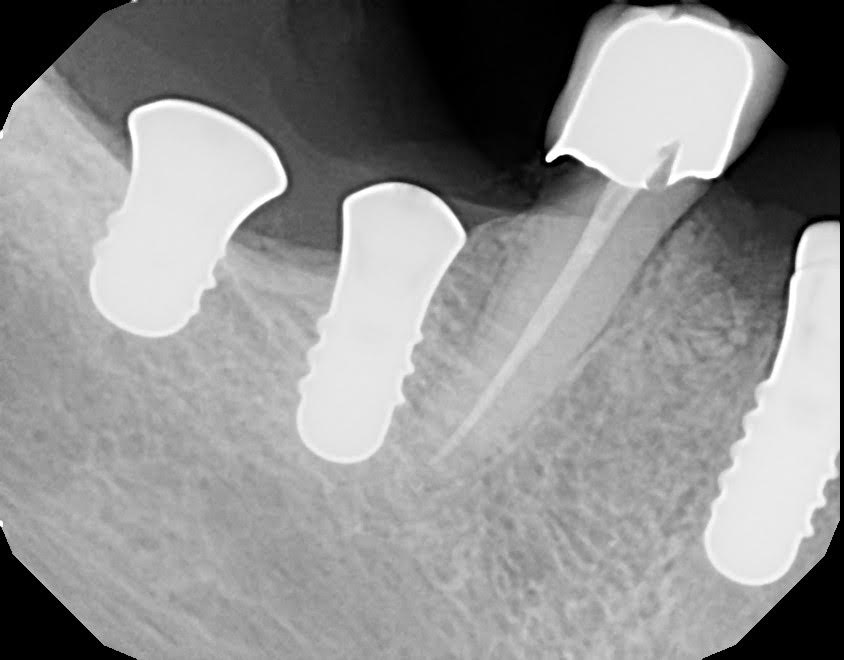
So now that I’ve checked the depth of the implant with my guidepins, I go and place the implant. It’s important to know your components. Straumann recommends 35Ncm, however with the Versah the bone tends to be harder with higher insertion torque. I keep my motor at a higher torque (Straumann’s loxim has a safety feature to break at 80Ncm, but I keep it still well below that).
I put the implant in. Then I take a PA and Pan. With anterior implants I usually find the PA is sufficient as long as clear from any vital structures.
Picture of the flap design I used for this case. Mid-tooth anterior and posterior. Gave me ample buccal and lingual wall visualization:
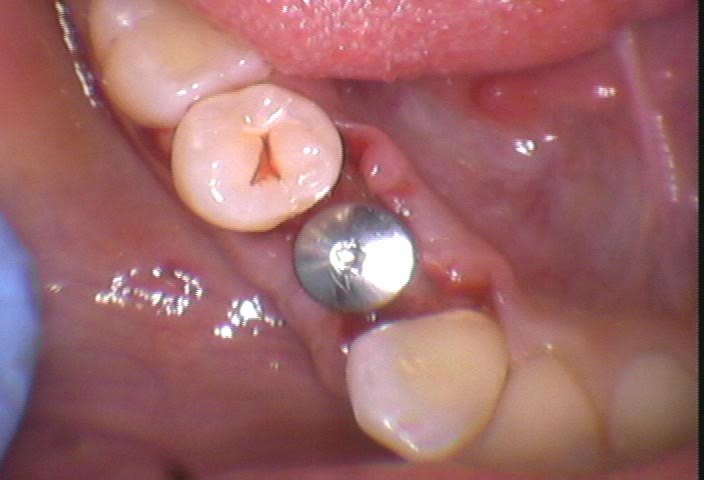
I flap until I can see the full buccal ridge and full lingual ridge. What I do is stop flapping mid-point on the adjacent teeth, and see if I can visualize what I need. If I need more, I flap more. Generally speaking at most I need to go to the distal / mesial of the adjacent teeth, but I aim for mid-tooth, as indicated with my stopping points here:
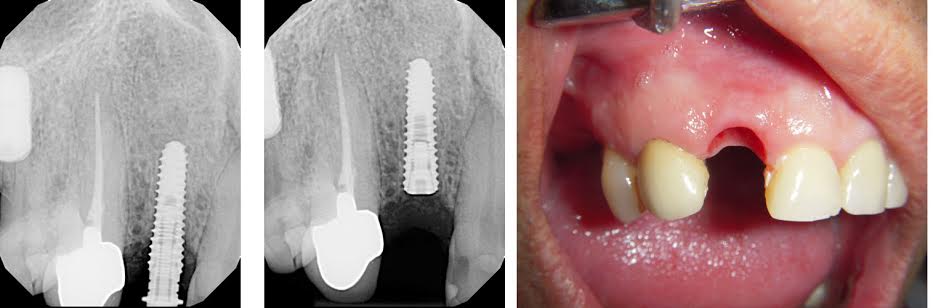
Took PA to verify implant placement
(Tip 5: when doing trickier cases, I often take a PA of the implant half-seated, so I can make some minor angulation changes without losing primary stability by seating it fully, then backing out. Stopping halfway down to take a PA works especially well with self-tapping implants like the Nobel Actives of Hiossen ETIII’s as there is more give with re-angulating)
Here is an example of stopping implant placement halfway to take a PA and changing angulation. Although I should have still burried this implant 1-2mm deeper. Hiossen 3.5x13mm:
Another example, Hiossen 3.5x13mm, but I should have stopped my implant placement even sooner to take the PA:
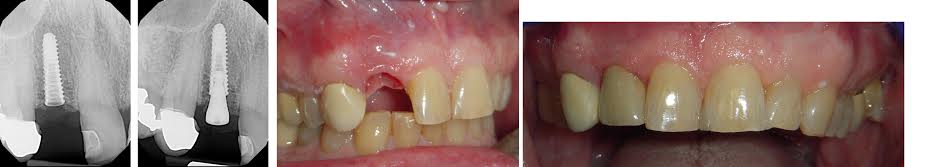
While the patient still won’t let me change the mismatched canine, here is the 3 year follow up on this particular case.
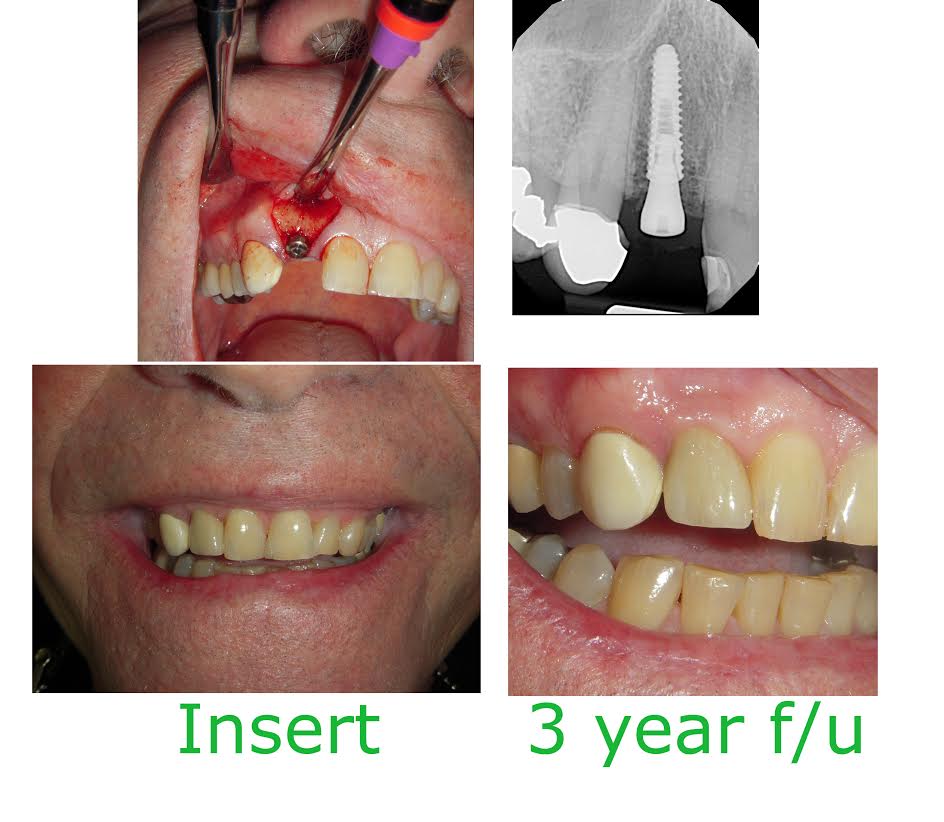
My assistant was STRUGGLING with her PA’s that day. I had a good idea of my distances and location of the IAN loop though, so I sutured and went ahead with the pan to minimize radiation for the pt
Ideally you want the whole implant + neighbouring teeth to show have not hit any vital structures. This is not a good x-ray and I talked w/ my assistant about this after the pt left.
As an associate, this can be tough to do (talk to an assistant about less than stellar performance). I have a section on how to approach this topic in my CE course Thriving as an Associate. You can learn more here (enrolment in the beta group closes at 11:59:59 PM Eastern time on April 15, 2018).
So here is the final PA that my assistant was struggling with. I knew my distances so knew I was a ways from the IAN, so I got her to take a Pan.
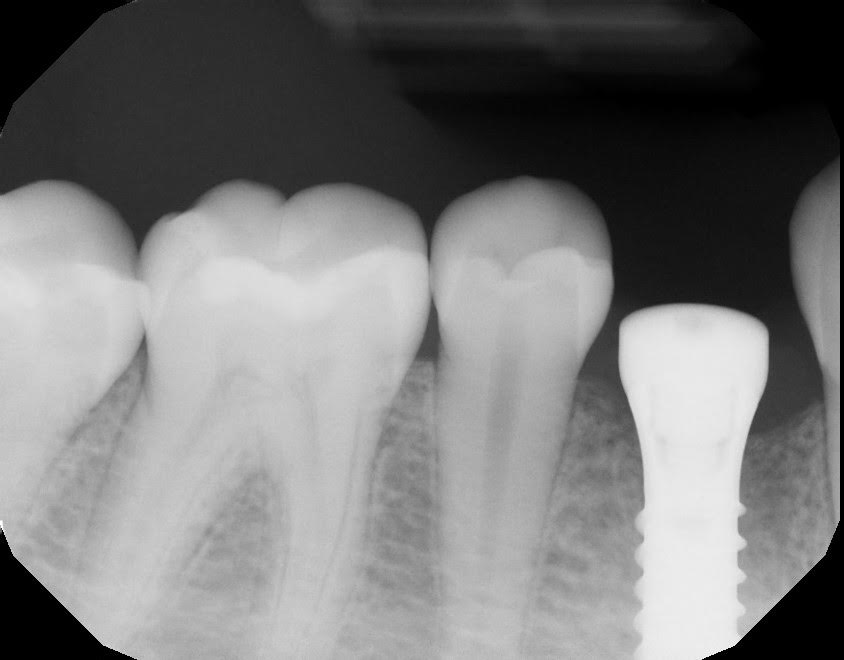
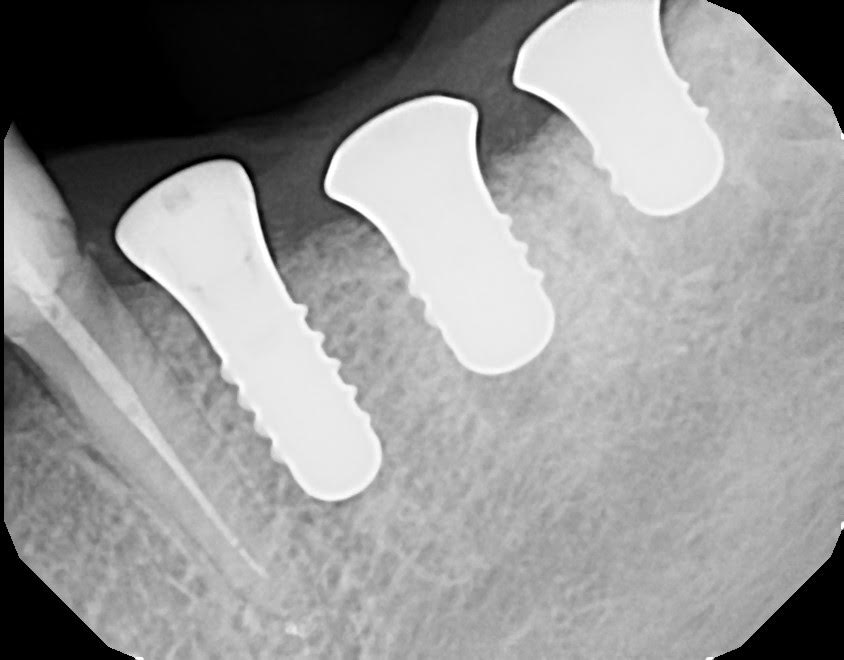
I personally like the Straumann tissue level implants. Two reasons. (1) The polished collar acts in a similar way to a platform switch – the junction is far away from the treated part of the implant, but more importantly, (2) the first threads of the implant are a ways down the body. So down the road, if there is bone loss, it is a lot easier to smooth and scale the roughened implant surface, compared to scaling and removing calculus from exposed threads on a bone-level implant. It’s purely a periodontal maintenance thought with me.
Would you want your hygienist to have to scale the above? Or have to smooth interproximal threads on this?
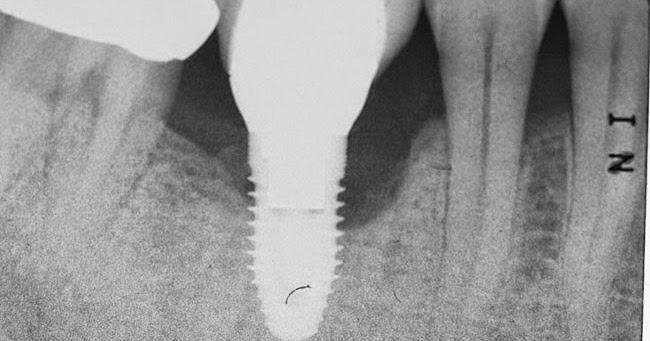
After placing the implant, I sutured. 4-0 PTFE. Hiossen has a good deal on their PTFE sutures currently. Make sure to talk to your periodontal and OMFS attendings, as they know more, but I love PTFE sutures. Stopped using silk 2 years ago. I find a monofilament, such as PTFE, the healing is a lot better than silk in my hands.
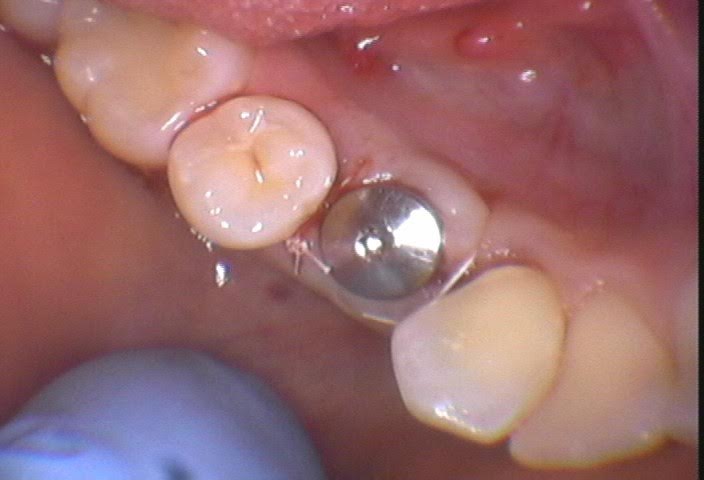
Two simple interrupted. Nothing fancy here. Good closure.
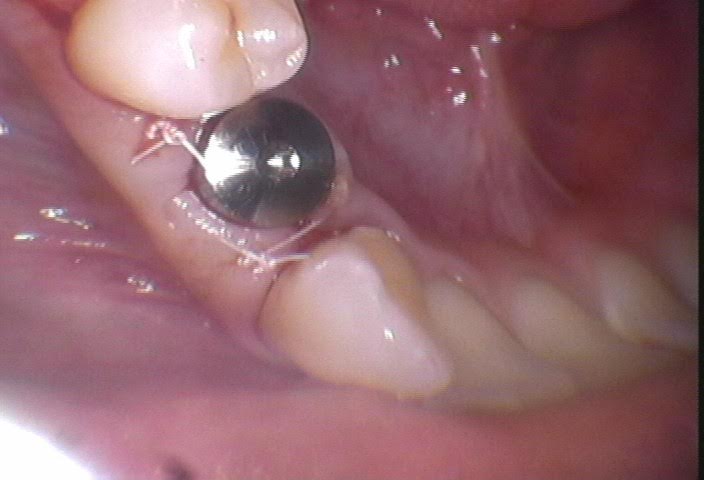
Final Pan
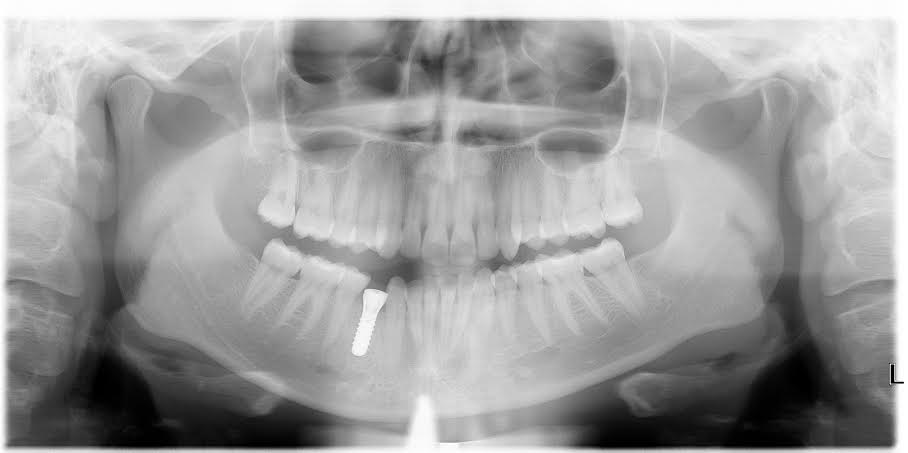
(efficiency) Tip 6: Take the pan before suturing if you anticipate moving the implant. If things are good, suture first and take the pan second as minimizing surgical time promotes quicker healing for the patient.
Scheduling
I like to book 90 mins for a 1-2 implants. I’m usually done placement in 45-50 mins, but it’s good to have that buffer in case something needs more attention or, more commonly, the pt is nervous and wants to talk, etc.
Plus as a GP you also have hygiene recall exams and other events that sometimes pull you away from your main treatment chair. So while I can do it consistently faster, 90 mins works for me. This is one of the few appointments I over-schedule time for. I want it to be a slam dunk for the patient experience.
Prescriptions
Pain meds and antibiotics: Give the pt 30 tabs of Ibuprofen 600mg, 12 tabs T3, a week’s worth of PenVK (healthy pt, quick surgery, other antibiotics I use are Amox, Amox/Clav, Z-pak, and Clinda depending on a variety of scenarios), her post-op instructions.
In future Helpful Dentist Insider’s email I will give you digital copies of the post-op forms I use
Followups
We see pt back 1 week for a 20 min wound check in the 2nd column (overflow room, booked against a light appointment w/ assistant time) and 2 weeks for a 20 min suture removal in the main treatment column. Sometimes, like on a lateral lift, I’ll leave selective sutures in for longer than 2 weeks, but it’s all based on how well the pt is healing.
So that’s how I do a routine private practice case in my office, laying out the step by step of how I do it.
For those who want some tips in implant impressions on multiple units here is a guide I wrote.
Tip 7: We have the NG fabricated at the same time as the dental implant, so it is more convenient for the patient. Implant crown + NG is delivered at the same visit.
We see the patient back 1 week later to check the bite, than at their next cleaning visit that is around the 6-month mark.
With larger cases we check the bite again at 1 w, 3 months, 6 months, and then yearly.
Here is how the case turned out. Patient was very happy.
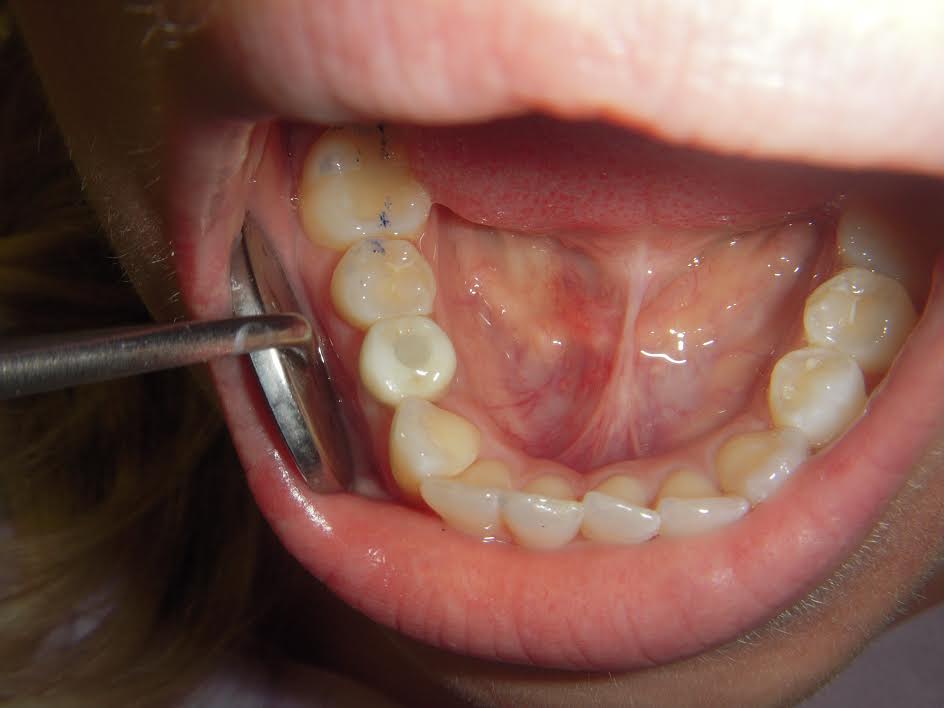
I hope this helps. Let me know if you have any questions
Dr. Greg (aka “The Helpful Dentist)